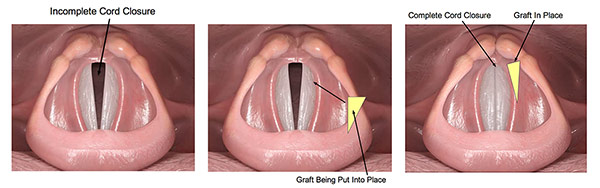
CAUSES OF VOCAL INJURY FROM THYROID SURGERY
Thyroid surgery may result in a weak voice for many reasons including:
- The breathing tube injuring the vocal cords
- The breathing tube weakening the vocal nerves
- Vocal nerve bruising during surgery
- Vocal nerve transection (cut) during surgery
- Worsening of a pre-existing weakness of a vocal nerve
- Complications with healing after surgery
Patients are often told to wait for spontaneous voice recovery. However, during this time, patients often have severe voice symptoms, making the waiting time difficult. Their voice problems may prevent them from returning to work, or make it difficult to socialize. For a professional voice user (singer, actor, etc), time spent waiting may severely limit career options.
VOICE PROBLEMS AFTER THYROID SURGERY
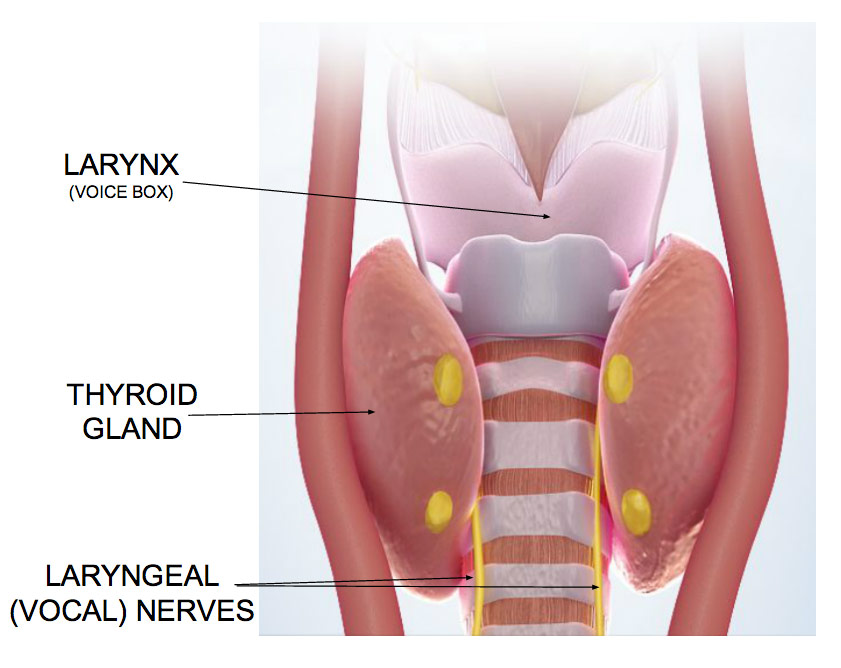
The thyroid gland is located in the neck, and sits on top of the vocal nerves. Because of this, surgery involving the thyroid gland can cause significant vocal damage.
THE BREATHING TUBE INJURING THE VOCAL CORDS
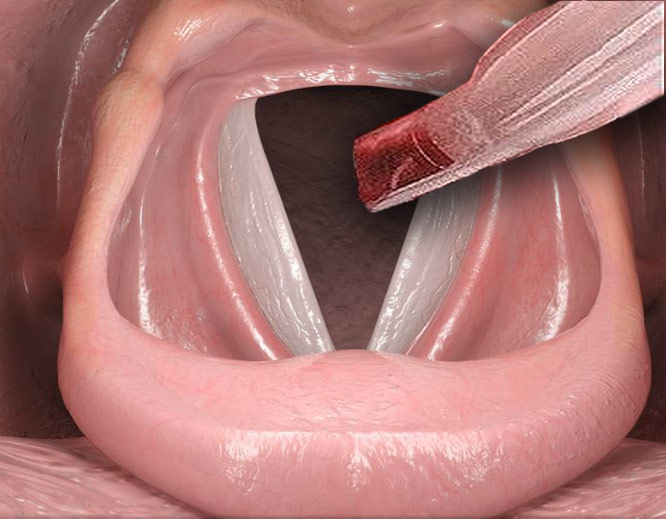
The breathing tube is placed between the vocal cords and contacts the vocal cords throughout the procedure. When it is placed, or if it shifts during surgery, it may injure the vocal cords.
THE BREATHING TUBE WEAKENING VOCAL NERVES

The breathing tube is placed between the vocal cords and contacts the vocal cords throughout the procedure. Prolonged surgery (i.e., more than one hour) may put pressure on the vocal nerves and weaken them.
VOCAL NERVE BRUISING DURING SURGERY

The thyroid gland sits on top of the major nerves involved in vocal function. To remove the thyroid gland, the surgeon has to elevate the gland off the nerve. This may bruise the nerve and make it dysfunctional.
VOCAL NERVE TRANSECTION (CUT) DURING SURGERY
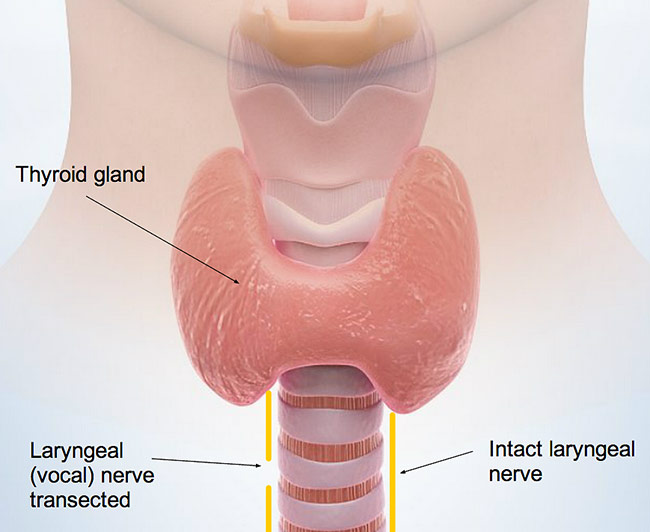
As the gland is lifted out of the patient, it may reveal that the vocal nerve was cut inadvertently during thyroid surgery.
WORSENING OF A PRE-EXISTING WEAKNESS OF A VOCAL NERVE
Sometimes patients may not know their vocal nerve is weak before they undergo thyroid surgery. The surgery then results in worsening of this weakness.
COMPLICATIONS WITH HEALING AFTER SURGERY
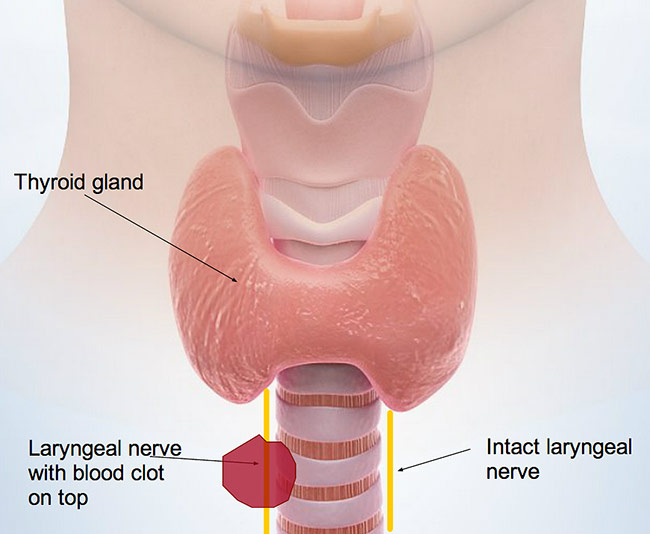
Complications after surgery, including a blood clot that can form in the wound bed, may put pressure on the vocal nerves, causing weakness.
Laryngoscopy for Diagnosis of Vocal Injury
LEFT VOCAL PARALYSIS
This video demonstrates a left vocal cord paralysis. The left vocal cord (on the right of the image) is not moving. This results in a large gap between the vocal cords, which results in a breathy and weak voice.
BILATERAL VOCAL PARALYSIS
Rarely, after neck surgery, both vocal nerves can be damaged. This results in inability to move both vocal cords. If the cords are stuck in the midline position, there may be significant difficulty breathing, as with the patient in this video.
Treatment Options
Depending on the details of your case, you may be a candidate for any one of several vocal treatment options.
VOICE THERAPY
Occasionally voice symptoms due to vocal injury from spine surgery are improved with voice therapy. Most patients should at least do a trial of therapy with a highly trained voice therapist (rather that a general speech therapist) before proceeding with any surgical options. Referral is provided by an expert laryngologist.
VOCAL CORD INJECTION
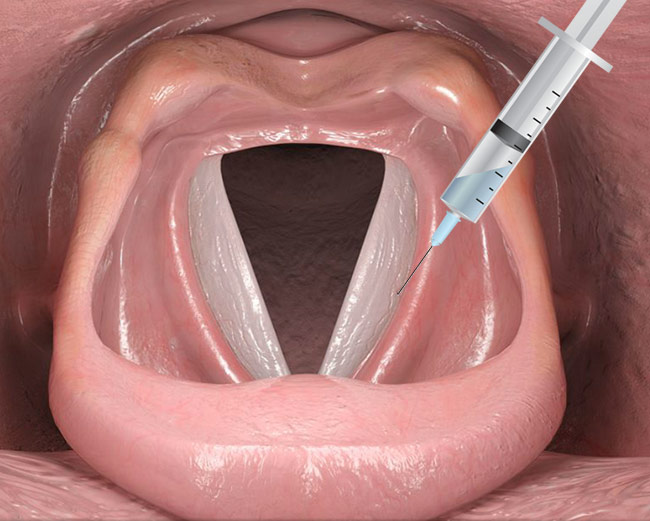
Vocal cord injection is performed when there is a vocal cord paralysis or partial paralysis (paresis). This procedure may be done under local or general anesthesia.It involves an injection into the side of the vocal cord, that fills the gap between the vocal cords by pushing the weak side closer to the strong side. There is minimal risk of a worsened voice.
THYROPLASTY
Thyroplasty is performed when there is a vocal cord paralysis or partial paralysis that results in a larger gap between the vocal cords or a gap in the back of the larynx (voice box). Large gaps and gaps in the back of the larynx respond better to thyroplasty than injection.
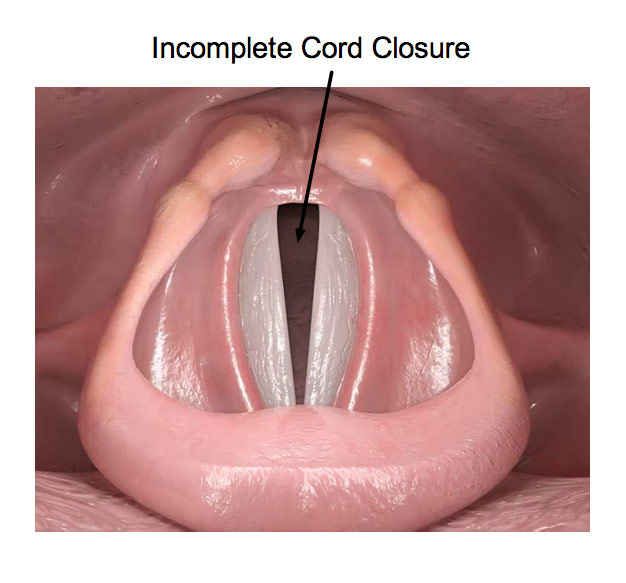
Thyroplasty involves implanting a material on the side of the vocal cord that pushes it closer to the strong side. This involves an incision in the neck that is closed by a plastic surgeon, to avoid cosmetic issues.